April 22, 2026
If you’ve ever felt guilty after a meal, found yourself obsessing over what you ate, or noticed a pattern of restricting and then overeating, you might have wondered: is this normal? Or is something more going on?
It’s a question we hear often, and honestly, it’s not always easy to answer.
The line between disordered eating and a clinical eating disorder isn’t always clear-cut. Both are real, both can cause real harm, and both deserve support.
This post breaks down the difference in plain, judgment-free language, so you (or someone you support) can better understand what’s happening and know when to reach out for help.

What Is Disordered Eating?
Disordered eating refers to a wide range of irregular or unhealthy eating behaviors and attitudes toward food. Behaviors that cause distress or interfere with daily life, but don’t necessarily meet the clinical criteria for a diagnosed eating disorder.
Here’s the important part: disordered eating is incredibly common, and much of it is quietly normalized by diet culture. You don’t have to be in a clinical crisis to be struggling.
Some common examples of disordered eating include:
- Chronic dieting or yo-yo dieting
- Labeling foods as “good” or “bad”
- Feeling guilt when eating the “wrong” ones
- Skipping meals or restricting food intake to compensate for eating more earlier
- Constant preoccupation with food, calories, or body size
- Feeling out of control around certain foods
- Rigid food rules that cause anxiety when broken
None of these experiences require a diagnosis to be worth addressing.
If your relationship with food is causing stress, that matters! And if you’re noticing patterns like emotional eating or the restrict-binge cycle showing up regularly, those are worth paying attention to, even if they feel “not serious enough” to mention.
Learn more in our blog post Understanding The Restrict-Binge Cycle: Why It’s Not About Willpower.
What Is an Eating Disorder?
Eating disorders are clinically diagnosed mental health conditions with specific diagnostic criteria. They go beyond irregular eating patterns and typically involve significant psychological distress, physical health consequences, and serious disruption to daily functioning.
The most common eating disorders include:
- Anorexia Nervosa: Characterized by severe restriction of food intake, an intense and often consuming fear of weight gain, and a distorted relationship with body image
- Bulimia Nervosa: Involves cycles of bingeing and purging (through vomiting, laxatives, or excessive exercise), often accompanied by deep shame and secrecy
- Binge Eating Disorder (BED): Recurrent episodes of eating large amounts of food, often rapidly and past the point of comfort, followed by feelings of guilt or loss of control — without purging behaviors
- Avoidant/Restrictive Food Intake Disorder (ARFID): Extreme food avoidance or selectivity that isn’t driven by body image concerns, often rooted in sensory sensitivities, fear of choking, or difficult past experiences with food
- Other Specified Feeding or Eating Disorder (OSFED): Eating disorder symptoms that cause significant distress, but don’t fit neatly into one of the above categories
Behind every one of these diagnoses is a real person doing their best to cope with something incredibly difficult.
Eating disorders are serious medical conditions. Not a phase, not a lifestyle choice, and not something a person can simply “choose” to stop.
They are among the most deadly mental health conditions and require specialized, compassionate care.

So What’s the Difference?
Think of disordered eating and eating disorders as existing on the same continuum, not as two completely separate categories.
Disordered eating sits on one end of the spectrum; clinical eating disorders on the other. But the line between them isn’t always fixed, and one can develop into the other over time like the visual below:
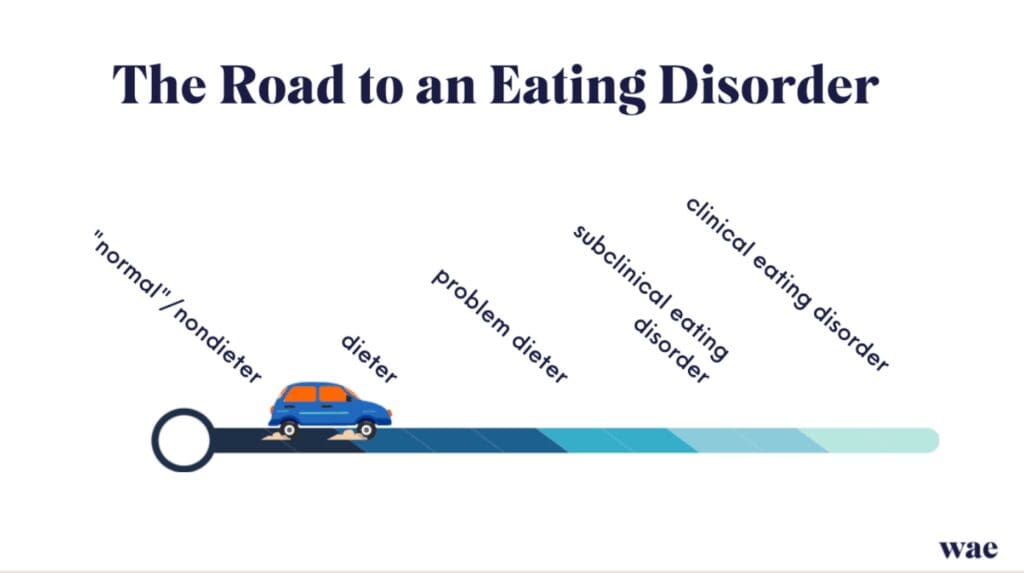
Here’s a quick side-by-side look:
| Eating Disorder | Disordered Eating |
| Requires a clinical diagnosis | Does not require a diagnosis |
| Specific diagnostic criteria must be met | Exists on a spectrum — no “threshold” required |
| Often involves significant physical health consequences | May not have visible physical symptoms |
| Typically requires a specialized treatment team | Also? benefits from professional support/team |
| Examples: Anorexia Nervosa, Bulimia Nervosa, BED, ARFID, OSFED | Examples: chronic dieting, guilt after eating, rigid food rules |
| Can develop from long-term disordered eating patterns | Can escalate into a clinical eating disorder over time |
The key takeaway: The difference isn’t about how much someone is suffering. Both ends of the spectrum can cause real pain, and both deserve real support.
Not sure where your experience falls? Our blog post Disordered Eating: Red Flags You Shouldn’t Ignore can help you get clearer on what to watch for.
The Role of Food Anxiety in Both
Whether someone is dealing with disordered eating or a clinical eating disorder, food anxiety is almost always part of the picture.
Food anxiety can look like:
- Dreading social situations that involve eating
- Spending significant mental energy planning or avoiding meals
- Feeling a wave of guilt or panic after eating something “off plan”
- Lying awake at night thinking about what you ate that day or what you’ll eat tomorrow.
If any of that sounds familiar, you’re not alone. This is more common than most people realize, and the data backs it up.
According to the National Eating Disorders Association, 28.8 million Americans will experience a clinical eating disorder in their lifetime. And that doesn’t account for the far larger number living with disordered eating, a 2023 review found that up to 22% of children and adolescents alone are affected.
These aren’t rare outcomes. They’re a predictable result of a culture that treats restriction as a virtue.
If food anxiety is taking up significant space in your daily life, whether or not it meets a clinical threshold, that’s meaningful information.
It’s a signal that your relationship with food could use some support.

When Should You Seek Support?
You don’t need to hit rock bottom or have a diagnosis, to prove that things are “bad enough.”
If your relationship with food is causing stress, that’s enough of a reason to reach out.
Some signs it’s time to bring in support:
- Food thoughts are taking up a significant amount of your mental energy
- Eating patterns are affecting your relationships, work, or daily life
- You feel caught in a cycle of restriction, guilt, or compensation that’s hard to break
- Mealtimes feel stressful more often than not
- You find yourself avoiding social situations because of food
- Someone close to you has expressed concern
You don’t have to be in crisis to deserve help. Reaching out early, before patterns become more entrenched, can make a significant difference in your recovery journey.
What Does Disordered Eating Recovery Look Like?
Recovery isn’t about eating “perfectly.” It’s about building a relationship with food that supports your life, instead of controlling it.
Working with a registered dietitian who specializes in disordered eating therapy can be a powerful part of that process.
A weight-inclusive, non-diet approach focuses on:
- Understanding the root of your food beliefs and where they came from
- Challenging rigid food rules and replacing them with flexibility
- Reducing food anxiety and rebuilding trust with your body
- Working through emotional eating patterns with curiosity instead of judgment
- Creating sustainable habits that support your wellbeing — without restriction or shame
Disordered eating recovery isn’t linear, and it looks different for everyone.
But with the right support, it is absolutely possible to reach a place where food feels neutral and enjoyable rather than something to manage or fear.
How We All Eat Can Help
At We All Eat Nutrition Therapy, we support individuals and families at all points on this spectrum, from those just beginning to question their relationship with food, to those working through a clinical eating disorder diagnosis.
We know that reaching out can feel like a big step, especially if part of you is still wondering whether what you’re experiencing is “serious enough” to warrant support.
Whatever you’re carrying around food right now, you deserve peace with food.
Our approach is weight-inclusive, non-diet, and centered on you, not a one-size-fits-all plan. We work with you to untangle food rules, build flexibility, and find a way of eating that actually fits your life.Ready to take the first step? Submit an appointment request here, we’d love to help.

The Bottom Line
The line between disordered eating and a clinical eating disorder isn’t always obvious, and that’s okay. What matters most is how food is affecting your life right now.
Wherever you are on the spectrum, your experience is valid. You don’t have to have a diagnosis to struggle, and you don’t have to struggle alone.